Insurers playing roughWhy do insurance companies play rough with legitimate claims? And, more important, what can you do if it happens to you?(Money Magazine) -- Are insurers more hard-nosed with claims than they used to be? Since the industry is regulated by the states, there are no national data to draw on. But the scattered state-level evidence suggests that insurers may be taking a harder line.
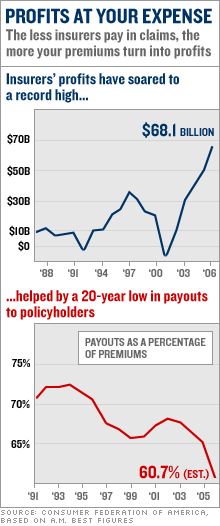 In Michigan, for instance, complaints against insurers are up 16 percent over 2001, while in Connecticut, justified complaints against health insurers (those considered to have validity by regulators) have risen more than 60 percent since 2000. Enforcement action is up too: In Texas last year the number of cases against insurers increased 21 percent compared with 1999. Current headlines, meanwhile, leave a strong impression. For starters, there's the ongoing Hurricane Katrina saga, in which companies like Nationwide, State Farm and USAA debate thousands of plaintiffs on such existential issues as whether the damage to the Gulf Coast was due to flooding, which typically isn't covered, or wind, which is. In California, meanwhile, Blue Cross recently settled more than 60 cases in which policyholders claimed their coverage had been unfairly voided, and regulators slapped both Blue Cross and Kaiser Foundation Health Plan with six-figure fines for wrongful rescissions. (The carriers say they're working with state regulators to improve their practices.) Against this contentious backdrop, it's ironic that insurers are thriving. Big public health carriers have been posting 20 percent-plus gains in earnings, and property/casualty companies (which cover, for example, autos and homes) are more profitable than ever. Or maybe it's not so ironic. A study this January by Robert Hunter, a former insurance commissioner of Texas, now the insurance director of the Consumer Federation of America, shows that property/casualty insurers are paying out less in claims relative to the premiums they collect than at any time in the past 20 years. That's partly due to smart underwriting and higher premiums, which have jumped 100 percent or more in some coastal markets over the past few years. But lower claims payouts also play a role. Hunter, along with a chorus of consumer advocates, attributes some of that to increasingly aggressive claims management across the industry. More bare knuckles in the claims department, more battles with consumers. Hardball with homeowners Don't ask Geoff Still about claims management. In October 2005, a hurricane nearly lifted the roof off his home in Coral Springs, Fla., drenching the interior with torrents of rain. Still, now 38 and the director of finance and operations at a local university, says he called his insurer, Universal Property & Casualty, the next day to report his loss. But it took four months, plus numerous follow-up calls and faxes with "Please Help Us" in 36-point type, to get an initial estimate. Meanwhile, mold spread through the house, and Still, his eight-year-old son, his five-year-old daughter and his wife Stacy, 34, then pregnant with their third child, had to move out. The insurer's first offer came in at $64,000, later upped to $94,000 - far less than the $175,000 in estimates Still had gotten for fixing the roof, replacing drywall and installing new floors. He turned down the offer and hired a lawyer. Shortly after, Universal sent his lawyer a check for $94,000, even though Still had rejected that amount as too low. At that point he had his lawyer file suit against Universal. As of late January, 15 months after the storm, Still and his family (including his new baby boy) are still living with his parents. "I believe 100 percent that they're purposely lowballing my claim," says Still. "They figure you have to take their offer because you need to move on." New tactics Universal's response to his theory is unknown, since the insurer did not return Money Magazine's calls. But it sounds right to Santa Fe plaintiffs attorney David Berardinelli. Berardinelli is the author of "From Good Hands to Boxing Gloves," a book based on some 12,500 PowerPoint slides that fell into his hands during a lawsuit against Allstate Insurance Co. The slides had been presented to Allstate between 1992 and 1997 by management consultant McKinsey & Co. as part of an overhaul (the Claim Core Process Redesign) of the insurer's claims handling process. Much of the presentation encourages Allstate to adopt a hard-nosed approach to claims. One typical slide picked from the book refers to taking a stricter stance on settlements: "Stand firm on final offer with no real negotiation." Another - and the inspiration for the book's title - distinguishes between the treatment to be accorded to customers who hire a lawyer to press for a higher payout and those who don't: The unrepresented get the "good hands" approach (settlements within 200 days or so); the lawyered get "boxing gloves" (resolution that could take three years or longer). Think of it as the Oliver Twist strategy: Accept the company's initial offer (which may seem more fair to Allstate than it seems to you ) and you'll get your money quickly. Ask for more and you may be in for a battle. And while the slides specifically deal with Allstate's auto division, Berardinelli and others familiar with the project contend the concept was applied to homeowners as well. The strategy outlined in the slides sounds much like the marching orders Shannon Brady Kmatz says she got when she was an Allstate claims adjuster. Kmatz, who left Allstate in 2000, says she felt under constant pressure to "fast-track" claims - that is, settle quickly for as little as possible. "We called it throwing them a bone," she said. "You offer $500 and hope they go away." She said she was also evaluated on how successful she was at convincing people to accept the company's offer rather than try to get more money by hiring an attorney. Adjusters who excelled at these goals, Kmatz says, were rewarded with free dinners and bonuses that could add up to a few thousand dollars a year. Kmatz provided evidence of such bonuses in a 2003 affidavit that is part of a class-action suit Berardinelli has filed against Allstate, and Money Magazine has reviewed those documents. Allstate wasn't the only insurer to ask management consultants to help revamp claims processing, say several former claims adjusters. McKinsey helped State Farm with the program known as ACE, or Advancing Claims Excellence, and Accenture advised Farmers Insurance, which had a claims program called ACME, short for Achieving Claims Management Excellence. (McKinsey and Accenture would not comment on their role, citing confidentiality.) All three insurers confirm the projects took place but deny that they were intended to help them shortchange policyholders in any way. "Ridiculous and completely false," says Allstate spokesman Michael Trevino. He points out that Berardinelli has an obvious interest in exaggerating the import of the slides to try to promote his book. And he says the company does try to settle claims quickly, but not at the expense of policyholders. State Farm and Farmers also reaffirm their commitment to paying what they owe promptly and fairly and point out that the projects in question ended several years ago, implying that whatever effect the consultants may have had on claims handling, it isn't relevant today. That may be, but it would be unusual for a business to hire a consulting firm with the intention of tossing out their work as soon as the M.B.A.s went home. Gary Fye, a claims consultant familiar with all three companies, agrees. "These practices continue today," he says. One thing is not in dispute: All three insurers have made startling progress in lowering their claims payout ratios since they engaged the consultants. At Allstate, claims paid fell from 87.2 percent of premiums charged in 1992 to 43.5 percent last year, according to the CFA's Hunter. At State Farm the ratio dropped from 77.5 percent in 1994 to 66.6 percent in 2005 (the most recent figure available), while at Farmers it fell from 74.7 percent in 2001 to 56.9 percent. Claims management certainly didn't account for all of the drop. But whatever the insurers are doing in that regard, it's working. More from the Money special report: How insurers can hold down payouts - and how to protect yourself Neutron bomb of health insurance: Suddenly not covered What you can do: Improve your odds of getting the policy benefits you expected |
|

