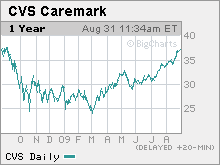
CVS Caremark: The one-stop health stock
It's a retailer. Wait, it's a health-care company. Actually it's both. And it's time for investors to realize that.
| MMA | 0.69% |
| $10K MMA | 0.42% |
| 6 month CD | 0.94% |
| 1 yr CD | 1.49% |
| 5 yr CD | 1.93% |
NEW YORK (Fortune) -- The controversy over health-insurance reform has cast a pall over usually robust health-care stocks. But even as that sector has lagged the S&P 500 this year, two subgroups have thrived: drug chains such as Walgreen, whose shares have jumped 24% since 2008, and pharmacy benefits managers (PBMs) such as Medco, up 30%.
So why isn't CVS Caremark (CVS, Fortune 500), which combines those two business lines, keeping pace? Sure, shares of the $87 billion corporation have risen a healthy 18% this year. But investors don't yet seem to understand the company, analysts say.
The market questions whether a drugstore chain, which has expertise in retail sales, can run a PBM, which negotiates on behalf of employers and insurance plans to purchase drugs from pharmaceutical companies. As a result, CVS's price/earnings ratio for the next 12 months is 13, while Walgreen's is 15 and Medco's is 20. That makes CVS, which is poised for strong growth, a bargain - no matter how the health-reform battle plays out.
CVS is typically viewed as a retailer, not a health-care company. In truth it's both. Based in Woonsocket, R.I., the business operates nearly 7,000 drugstores. The company was reconfigured with the $26.5 billion acquisition of Caremark Rx, the giant PBM, in 2007.
Over the past five years CVS has increased earnings by an average of 20% each year, compared with an industry average of 8%. Analysts expect it to boost profits 16% annually over the next five years, compared with Walgreen's (WAG, Fortune 500) 13% and Medco's (MHS, Fortune 500) 17%.
CVS looks particularly attractive if you employ the legendary investor Peter Lynch's favorite metric: comparing a stock's P/E ratio with its growth rate. The so-called PEG ratio is a way to gauge the potential to buy growth at a bargain price (a lower number is better). In this case, CVS scores 0.84, compared with Walgreen's 1.19 and Medco's 1.18.
How would reform affect CVS? Details have yet to be ironed out, but policymakers have zeroed in on a couple of goals: improving access to insurance and cutting costs. Unlike, say, Big Pharma and managed-care companies, CVS is likely to benefit.
"Increased coverage is generally good for CVS," says Scott Mushkin, an analyst at Jefferies & Co. If more people have insurance, CVS and Caremark get more customers. Lower drug prices would initially hurt sales, Mushkin says. But because the company's retail and PBM operations buy drugs wholesale and sell them to consumers and employers, they would ultimately benefit from the higher volumes that come with cheaper medicine.
Regardless of what happens in Washington, macro trends - an aging population buying more drugs each year - favor CVS. Pharmacy sales were up 17% last quarter, and the company also managed to sustain growth in sales of products like cigarettes and soft drinks over the past year. Its average ticket, or amount spent per visit, has gone up.
CVS is a best-in-class retailer, says Meredith Adler, an analyst at Barclays Capital. "They didn't just do one thing - it's a long list of achievements," she says.
Adler points to CVS's store layout, which she says is more comfortable than rival Walgreen's "claustrophobic" design. She also says customers love the CVS ExtraCare card, which grants rewards, and its growing lineup of private-label products.
The company has also improved its pharmacy technology and built hundreds of MinuteClinics, in-store health-care centers that treat common ailments. These services lure customers into stores, where, CVS hopes, they'll fill their shopping baskets, bumping up retail sales.
Where CVS has been less successful is in its PBM business. Caremark's growth since the merger has been disappointing. The PBM lost a $1.4 billion contract to Medco last year, for example, and has had to renegotiate deals at lower prices. Caremark recently posted a strong quarter, but profits are increasing more slowly than those of competitors, analysts say, and CVS needs to demonstrate that the vertically integrated business model makes sense.
Some think the model is already working. "It's a multifaceted strategy that takes advantage of the strengths of both companies," says Steven Halper, an analyst at Thomas Weisel Partners. "They can exploit the PBM in order to drive traffic."
He points to an innovative initiative called Maintenance Choice, which gives Caremark customers the option of receiving discounted 90-day prescriptions via mail or in CVS stores. CVS announced last quarter that 270 payers, which include insurers and employers, have signed up for the program. Some 25% of the new contracts last quarter are new to Caremark. That's a sign, CEO Tom Ryan said on a recent earnings call, that big customers like the bundled option.
Now CVS has to persuade investors to buy the package deal too. Adler is sold. "I don't buy the argument that they're a retailer who doesn't understand the PBM business," she says. "They didn't get where they are by accident." ![]()
-
 The retail giant tops the Fortune 500 for the second year in a row. Who else made the list? More
The retail giant tops the Fortune 500 for the second year in a row. Who else made the list? More -
 This group of companies is all about social networking to connect with their customers. More
This group of companies is all about social networking to connect with their customers. More -
 The fight over the cholesterol medication is keeping a generic version from hitting the market. More
The fight over the cholesterol medication is keeping a generic version from hitting the market. More -
 Bin Laden may be dead, but the terrorist group he led doesn't need his money. More
Bin Laden may be dead, but the terrorist group he led doesn't need his money. More -
 U.S. real estate might be a mess, but in other parts of the world, home prices are jumping. More
U.S. real estate might be a mess, but in other parts of the world, home prices are jumping. More -
 Libya's output is a fraction of global production, but it's crucial to the nation's economy. More
Libya's output is a fraction of global production, but it's crucial to the nation's economy. More -
 Once rates start to rise, things could get ugly fast for our neighbors to the north. More
Once rates start to rise, things could get ugly fast for our neighbors to the north. More








